Biography
Interests
Mauricio Cataldo Muñoz1*, Eduardo Fuentes Morales1, Gianella Aceituno Benvenuto1 & Marco Higueras Contreras2
1Department of Traumatology and Orthopedic Surgery, Hospital Clinico IST Viña del Mar, Chile
2Department of Physical Therapy, Hospital Clinico IST Viña del Mar, Chile
*Correspondence to: Dr. Mauricio Cataldo Muñoz, Department of Traumatology and Orthopedic Surgery, Hospital Clinico IST Viña del Mar, Chile.
Copyright © 2021 Dr. Mauricio Cataldo Muñoz, et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
To present a retrospective descriptive study reviewing the postoperative results, following its clinical
and rehabilitation processes, to compare the results obtained with existing evidence, with regards
to the surgical technique used and the use of heel lifts in the postoperative rehabilitation process.
A retrospective descriptive study was conducted on adult patients with a clinical diagnosis of
Achilles tendon rupture operated between 2012 and 2020. Clinical and epidemiological data were obtained. All underwent percutaneous repair with the Dresden instrument by the same traumatologist
specialized in foot and ankle.
The study included 79 patients between the ages of 20 and 74 years of age. The clinical diagnosis
of Achilles tendon rupture was confirmed in all participants using the Simmonds triad. Data were
collected regarding the manner of injury, time before returning to sports and work, evaluation
of the post-operative functional outcomes using AOFAS, user satisfaction, and postoperative
complications.
Percutaneous surgery with the Dresden instrument has been shown to have good results in the
short, medium, and long term. We propose a modification of the original surgical technique by
using a dynamic and a static suture, which resulted in positive levels of satisfaction, without the
affected Achilles tendon re-rupturing. We present the possibility of using silicone heel lifts with
lower elevation than that described in the literature to obtain good long-term functional and
anatomical results.
Abbreviations
AOFAS = American Orthopedic Foot and Ankle Society Ankle-Hindfoot Score
Introduction
The Achilles tendon is the strongest and largest tendon structure in the body. It is the joint tendon of the
gastrocnemious and soleus muscles, but it may also have a small contribution from the plantaris [1-2]. It
is the tendon that is subject to the highest loads in the body, with loads of up to ten times the body weight
during activities such as jogging and jumping [3]. As a remarkable part of its anatomy, it presents a hypovascular
zone demonstrated by the angiographic studies of Lagergren and Lindholm in 1959, which is
located approximately 4-6 cm above its insertion with the calcaneus bone, where approximately 75% of the
ruptures of this tendon occur [4-6].
Acute rupture of the Achilles tendon is one of the most frequent injuries in adults, which in recent years has seen a progressive increase, with incidences ranging between 7 and 40 per 100,000 inhabitants [7,8]. It is predominant in males and according to some analyses, it is more frequent among men between 20 and 39 years old who practice some type of sport [8,9].
Acute Achilles tendon ruptures are not only caused by sudden excessive load but may also be the terminal process of a chronic degenerative condition, a manifestation of a systemic disease, or even a side-effect of the use of anabolic steroids, injectable corticosteroids and, the use of fluoroquinolones [10-12].
There is no gold standard when it comes to the treatment of a ruptured Achilles tendon, and there are both orthopedic and surgical alternatives to treat this injury [13,14].
We propose that the minimally invasive approach using the Dresden instrument is a surgical technique that has advantages in the immediate postoperative period, reducing the risk of wound infection [15], and presents biomechanical advantages by decreasing the time in the return to work and sports, compared to the other repair techniques [16,17].
The objective of this study is to characterize the group of patients operated on using the minimally invasive surgical technique with Dresden instrument, describe the surgical technique used, the rehabilitation protocol followed and compare the results with the existing literature.
Materials and Methods
A retrospective case series study was conducted. We included adult patients 18 years of age or older operated
on between February 2012 and December 2020 who were clinically diagnosed with Achilles tendon rupture
using imaging correlation. Patients were operated at Hospital Clínico IST, by a single traumatologist
specialized in foot and ankle. Those with a diagnosis of tendon re-rupture were excluded.
Patients underwent Achilles tendon repair surgery, using the percutaneous technique with the Dresden instrument. At the time of discharge, all patients left with an equinus cast.
Patients were monitored 14 days after surgery, for clinical evaluation and removal of stitches and cast. They were fitted with an orthopedic weightbearing boot. After this evaluation, patients were sent to kinesiotherapy which consists of six independent phases for rehabilitation, following the protocol established by the hospital’s foot and ankle team. A monthly medical check-up was carried out by the same traumatologist who performed the surgery, until the patient was able to participate in sports again.
Epidemiological data were recorded that allowed the description of the study population, complications, postoperative functional outcomes calculated by AOFAS [18] and user satisfaction.
This study had the informed consent of patients and was presented and approved by the ethics committee of the Hospital Clínico IST.
Results
A total of 79 patients were included, 74 men and 5 women. Patients were between the ages of 20 and 74,
with an average age of 41. Forty-two patients injured their right Achilles tendon and 37 patients the left.
All patients exhibited the Simmonds triad [19], which consists of a positive Thompson test, a positive
Matles test and, a palpable gap. All patients also underwent imaging studies, either ultrasound or magnetic
resonance imaging to corroborate the clinical diagnosis.
With regards to the mode of injury, 60 patients were injured playing soccer and the other 19 were injured by other means: 9 spontaneously, 5 jogging, 2 playing basketball, 2 playing volleyball and 1 by direct damage.
Regarding time until the return to sports, of the 79 patients, 74 performed physical activity and 5 were sedentary before the rupture. A person who performed physical activity was considered to be one who performed at least 150 to 300 minutes of moderate-intensity aerobic physical activity, or at least 75-150 minutes of vigorous-intensity aerobic physical activity, according to the latest update from the World Health Organization (WHO) [20,21].
Of the 74 patients who performed physical activity, 15 did not resume sports activity, stating the main cause to be fear of the rupture of their contralateral Achilles heel. Fifty-nine patients resumed their sports activity in a reasonable time, with an average of 206 days.
Regarding the return-to-work time, of the 79 patients, 4 patients were retired and 3 were students. Of the 72 patients who were in the workforce, they returned to their activities, on average 67 days after surgery.
An evaluation of the postoperative functional outcome yielded an average AOFAS score of 99.89 out of 100.
Regarding user satisfaction, 77 patients expressed complete satisfaction and 2, satisfaction with minor reservations.
There were 2 postoperative complications in patients with underlying comorbidities; one was a wound dehiscence and the other a deep vein thrombosis.
Surgical Technique
The patient lies in a prone position, leaving the feet at the edge of the table. Subsequently, the location of the
rupture and the incision are marked.
An incision of approximately 2cm in length, less than 10cm from the upper edge of the calcaneus towards the proximal on the medial side is made under sterile conditions.
The fascia of the leg is opened, and Dresden instruments are inserted, which are palpated subcutaneously in the most distal area of the tendon. It should be noted that the peritenon is not opened. A needle with orthocord suture thread is inserted percutaneously through holes in both instruments and the strands are secured through the incision area. The same procedure is performed again at a different level than the previous suture.
The first strand is fixed to the muscular plane using two continuous stiches made with an eyeless suture needle providing enough tension to leave the ankle in the same equinus as the contralateral foot (dynamic suture). Two simple stiches are made with the second strand and tied between both ends of the suture, without creating greater tension than the tendon already had (static suture).
The area is cleaned with physiological serum and closed with sutures in two planes, using vycril 3-0 sutures subcutaneously and ethylon 3-0 for skin closure (Figure 1).
A: Patient in prone position, B: Skin marking of the upper edge of the calcaneus and the gap of the left Achilles tendon; C: Dresden instruments are inserted, and eyeless suture needle is used to stitch; D: The ends of both sutures are secured through the percutaneous approach; E: The ends are knotted in the area approaching the muscular plane; F: Operative suture of wound.
Rehabilitation Protocol
The foot and ankle team of the Hospital IST jointly developed a post-surgical management protocol for
patients operated on for ruptured Achilles tendon. This protocol was used as part of the follow-up and
rehabilitation process of the patients studied and consists of six independent phases (Figure 2).
The first phase is from the postoperative period, until the second week after surgery. At this stage, patients use Canadian crutches to move around and are instructed not to bear weight with the affected limb. The second phase is between the second and fourth week after surgery. At this stage, light weight bearing is allowed using an orthopedic boot with interior enhancement, maintaining the crutches to assist mobility.
The third phase takes place between the fourth and sixth week, where shoes with heel lifts may be worn and, there is independent walking and full weight bearing. In the fourth phase, between the sixth and eighth week, the heel lifts in the footwear are progressively removed.
Phases five and six, correspond to the return to work and sports respectively. The objective is to return to work from the 8th week onwards and return to sports activity from week twenty-four onwards.
Discussion
There are many variants of rehabilitation protocols in patients who have been diagnosed with acute rupture
of the Achilles tendon. In general, most of them seek to initially immobilize the ankle in equinus, with no weightbearing for the first two weeks and then continue with the rehabilitation guidelines, with progressive
weightbearing and decreases in equinus [22,23].
The reasoning for placing the ankle in an equinus position after surgery, is to facilitate contact between the repaired ends of the tendon and thereby favor healing and reduce immediate post-operative tension [24,25]. However, there is no consensus regarding the degree of equinus or level of elevation that the wedges or lifts must have to achieve this goal. In fact, there is still discussion in the literature about the optimal degree of equinus in postoperative immobilization.
In this study, the patients observed, used a Walker orthopedic boot with 2 silicone heels superimposed on each other inside, which provided an effective elevation of 1.65cm, based on the radiographic record of a male patient, weighing 70 kilos, weightbearing with 2 heel lifts in a Walker boot (Figure 3).
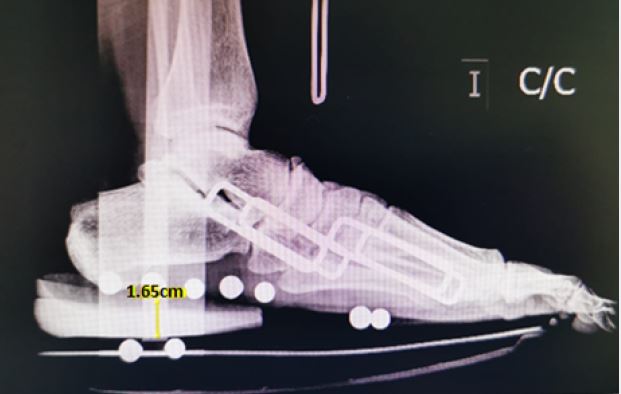
This value is far from the three cm with 20° angulation described in the literature that is used with progressive removal of 1cm [26-28]. Despite this, after a follow-up between 6 months and 9 years, with an average of 4 years, in 100% of the cases reviewed none of the affected tendons re-ruptured.
It is important to mention the above, since the use of these heel lifts has the advantage of being more affordable for the pubic and more readily available, compared to the lifts that are made to order. In addition, they are easier to handle and incorporate into different types of footwear, which makes it more likely that patients will adhere to instructions for postoperative care. This is also important considering that due to the current COVID-19 pandemic, access to certain orthopedic items has been limited, especially those that must be made-to-order. Having a mechanism that is simple to use and easily accessible is a considerable advantage.
In relation to the surgical approach, it should be noted that using the percutaneous repair technique with the Dresden instrument, the first stitch was always fixed to the muscular plane, leaving an amount of tension that would allow the ankle to be left in the same equinus as the contralateral ankle. This suture will be called dynamic, since it is the one that will provide the tension to the repair technique.
The second stitch, which is performed with the second strand would be a static suture, which does not aim to increase the tension already provided by the dynamic stitch. The above was done in this way to avoid producing greater tension than necessary so as not to interfere later in the rehabilitation process and thereby reduce the additional rigidity that could be caused with an excess of tension in the suture caused by an attempt to over secure the suture.
As a research group, we propose that more studies should be carried out to establish the real impact of the aforementioned factors in terms of caring for patients who suffered acute rupture of the Achilles tendon and were treated with a minimally invasive approach.
We leave open the discussion about these topics, which could eventually mean making the rehabilitation process easier and more accessible after surgery.
Conclusions
Percutaneous surgery with the Dresden instrument to repair ruptures of the Achilles tendon has been shown
to have good results in the short, medium, and long term.
We propose a modification of the original surgical technique using a dynamic and static suture, which yielded user satisfaction of almost all patients and did not have any re-rupture of the affected Achilles tendon.
It is important to consider that there are currently differences in postoperative care and protocols regarding rehabilitation. Among them, in this study we propose the advantage of utilizing silicone heels with lower elevation than that described in the literature to provide lift, which has very good functional and anatomical results in the long term.
Acknowledgements
None
Conflicts of Interests
The authors declare that they have no competing interests in this article.
Bibliography