Biography
Interests
Carlo Lazzari1*, Thimmaiah Rajanna1, Abdul Nusair1 & Marco Rabottini2
1Department of Psychiatry, Fieldhead Hospital, Ouchthorpe Lane, Wakefield, United Kingdom
2Centre for Neurosciences, International Centre for Healthcare and Medical Education, Bristol, United Kingdom
*Correspondence to: Dr. Carlo Lazzari, Department of Psychiatry, Fieldhead Hospital, Ouchthorpe Lane, Wakefield, United Kingdom.
Copyright © 2018 Dr. Carlo Lazzari, et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
The authors of the current article report on recent studies about the thinkable contribution of generalized sepsis and postoperative complications as hypothetical causes of Alzheimer Disease (AD) and psychosis in a vulnerable population. Author’s hypotheses have been supported by a clinical case in their psychiatric hospital that developed AD and psychosis after generalized sepsis and a major surgical operation.
Abbreviations (if used)
ACPAs - Anticyclic Citrullinated Peptide Antibodies
AD : Alzheimer’s Disease
ATF : Alzheimer Triggering Factor
BBB : Blood-Brain-Barrier
LPS : Lipopolysaccharide
PIPOAD: Post-Infection-Post-Operative-Alzheimer Disease
Short Communication
There is growing evidence that inflammation of the brain could be a cause of cognitive decline after the
activation of glial cells producing a substance called lipopolysaccharide (LPS), probably the principal
responsible for dementia found after diffuse systemic infections in animal models [1-3]. It is not clear
if the inflammation of the brain with the release of LPS after generalized sepsis could be a trigger or a
consequence of Alzheimer’s Disease (AD) with LPS altering the function of cerebral neurons and microglia
[4,5]. A meta-analysis suggests the contribution of neuroinflammation in mild cognitive impairment that
subsequently might progress to AD [6]. The authors of the current research already reported about a case
of a lady of age 64 who developed for the first time an irreversible cognitive decline with symptoms of
AD and psychosis after a major systemic infection and an extended operation for perforated duodenal
ulcer causing pneumoperitoneum [7]. The authors of the current study refer to this presentation as Post-
Infection-Postoperative-Alzheimer-Disease or PIPOAD. Studies report cases of the decline of cognitive
functions after significant surgery which can have a short- or long-term progression and can affect memory,
concentration, verbal fluency, and social skills; the likely cause is neuroinflammation triggered by surgery [8].
Other studies suggest the possibility of counteracting neuroinflammation leading to AD in mice with the use
of doxycycline antibiotic and thinkable application also in humans due to its power to cross the blood-brain
barrier [9]. Our clinical case brings to some speculative hypothesis about the effect of neuroinflammation on
the brain and as a possible cause of dementia and psychosis. Our case study is consistent with recent theories
which link neuroinflammation and postoperative complications to brain diseases, including dementia and
psychosis. In the PIPOAD the authors speculate the existence of an Alzheimer Triggering Factor (ATF)
[7,10] probably generated by a collection of factors that might be successive to systemic infection and/
or significant postoperative events following total anaesthesia. For instance, products of cellular lysis with
neurotoxic effect can trigger noxious events altering the blood-brain barrier (BBB). Products from cellular
lysis (with the release of lysosomes) and/or bacterial walls during sepsis or major surgeries can alter neuronal
and glial cell permeability when the microorganisms are already inactive after antibiotics and cross the
BBB. Lipopolysaccharide could act directly on cerebral neurons and glial cells in activating a cascade of
irreversible processes (ATF) conducive to irreversible cognitive decline and psychopathologies. The other
hypothesis of the authors of the current article is that infections and postoperative complications might both
activate circulating macrophages stepping into the BBB and initializing a process of phagocytosis targeting
neuronal and glial cells of the brain. In this case, macrophage lysosomes are accountable for the process [11].
The progression would be gradual or generalized (Figure 1) with:
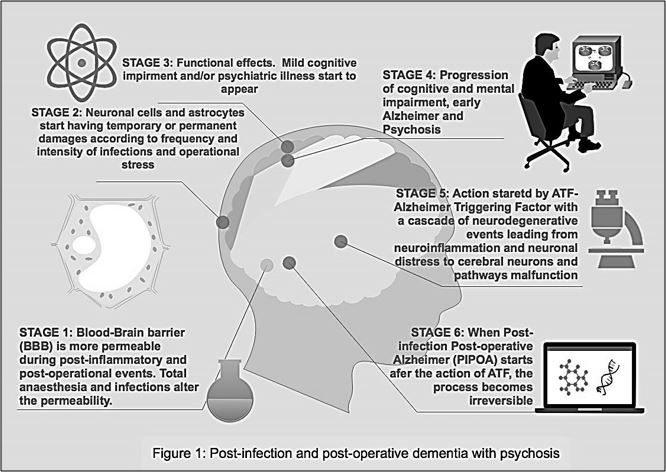
Stage 1: Generalized sepsis or major postoperative complications could alter blood-brain-barrier (BBB)
with the support of pathogens (e.g. bacterial, viral or cellular neurotoxins).
Stage 2: Pathogenic factors overcoming BBB might target neuronal cells or cerebral pathways.
Stage 3: Initial mild cognitive impairments in the post-infection or postoperative period.
Stage 4: Cognitive impairments and psychiatric symptoms become more apparent and long-standing.
Stage 5: A hypothetical Alzheimer Triggering Factor (ATF) generates an irreversible process. ATF could be
a group of processes like neuroinflammation, altered cerebral endothelium, increased cerebral neuronal loss,
bacterial or viral neurotoxins, products of cellular or bacterial lysis, and activated macrophages.
Stage 6: Increased and possibly irreversible cognitive and psychiatric impairment in PIPOAD not necessarily
produce delirium. The initial stages of cognitive and mental decline appear in clear consciousness to indicate
that the sensorium might not be altered during the initial stages.
In conclusion, PIPOAD could be initially reversible such as when a person suffers from delirium or altered consciousness during generalized sepsis. Afterwards, the process tends to become irreversible as ATF has a cascade effect.
Bibliography

Hi!
We're here to answer your questions!
Send us a message via Whatsapp, and we'll reply the moment we're available!