Biography
Interests
Suleiman I. Sharif1*, Danah S. Abbas2, Dana M. Husseyan2, Esraa Al Assadi2 & Rubian S. Sharif2
1Department of Pharmacy Practice & Pharmacotherapeutics College of Pharmacy, University of Sharjah, United
Arab Emirates
2Department of Pharmacology, Faculty of Medicine, University of Benghazi, Libya
*Correspondence to: Dr. Suleiman Ibrahim Sharif, Department of Pharmacy Practice & Pharmacotherapeutics, College of Pharmacy, University of Sharjah, United Arab Emirates.
Copyright © 2020 Dr. Suleiman Ibrahim Sharif, et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
The problem of bacterial resistance is worsened by the irresponsible utilization of antibiotics.
The present study aims at evaluating the knowledge of pharmacy students about various aspects of
antibiotics’ storage and use and bacterial resistance.
This is an anonymous questionnaire- based cross-sectional study. The survey was designed with
close ended questions and pre-piloted for face validity by distributing it to pharmacy students of
at the University of Sharjah-United Arab Emirates. The survey was distributed to a total of 264 students. The data was analyzed using SPSS version 20 and chi square test was used to determine
the level of significance of responses at p< 0.05.
The response rate was 91.3% with the majority (198, 82.2%) of respondents being females, Arabs
(230, 95.4%) and with parents of non-health care profession (182, 75.5%). About two thirds students
have had used antibiotics in the last year and they read the instruction leaflet. High percentages of
all students use antibiotics for fever, colds and sore throat, keep leftover antibiotics and use them
without medical consultations. More senior than junior students know that misuse can lead to
resistance and antibiotics are effective against bacteria but not viruses.
Senior students seem to have a higher but not ideal level of knowledge of antibiotics and bacterial
resistance than junior students. It is of importance to focus on interventions that enhance educational
courses for pharmacy as well as students of other colleges of health sciences as future health care
providers in addition to continuing educational programs for practicing health professionals.
Introduction
Antibiotic medications are widely applied in the treatment and prevention of infections. They may either
kill or inhibit the growth of bacteria; however, a major problem is arising that represents one of the biggest
threats to global health. This is attributed to self-medication and irrational use of antibiotic [1]. The problem
of resistance is worsened by the irresponsible practice of taking antibiotic without the advice of a physician
and also the use of leftover medicines stored at home and sharing antibiotics with family members [2]. It
has been argued that the prevalence rates of antibiotic use without prescriptions in UAE are considered high
and are due to the lack of enforcement of laws and regulations which would otherwise prohibit this practice
[3].
Irrational use will certainly lead to antibiotic resistance which can affect any one, of any age, in any country [4,5]. Emergence of resistant strains of microorganisms occurs when bacteria changes to protect itself from antibiotics [6]. It occurs naturally, but misuse of antibiotics in humans accelerates the process of emergence of resistant bacterial strains and the problem is enhanced by easy access to antibiotics. The problem although cannot be prevented, it can be tremendously reduced [7]. Several practices represent misuse of antibiotics such as unnecessary over-prescribing, under prescribing, patients not finishing the entire antibiotic course, overuse of antibiotics in livestock and fish farming, poor infection control in health care settings, poor hygiene and sanitation, unnecessary antibiotic prescribing, the slow progress in developing new antibiotics, antibiotic prescribing for non-bacterial infections, patient demands on physicians to prescribe antibiotics and self-prescribing. However, inappropriate prescribing of antibiotics by the physicians is the most important recognized factor [8]. Moreover, lack of awareness on rational use and self-medication with antibiotics has also been identified as major factors for the development of antibiotic resistance [9]. Antibiotic use is highly prevalent, with statistics [10] estimating a 66% global rate of antibiotic use. Purchase of antibiotics without a prescription is estimated to count for 50% world-wide [11]. Considering the importance of this health issue, the present study was carried out to evaluate the knowledge, attitude and practice of pharmacy students about rational antibiotic use and emergence of bacterial resistance.
Materials and Methods
Inclusion criterion in the present study applies to pharmacy students at the University of Sharjah. The
targeted sample includes first, third and fifth year students. Sample size was calculated using online Raosoft
calculator.
This study was conducted at the College of Pharmacy, University of Sharjah during the period 1st April to
30th June, 2019.
An anonymous cross sectional questionnaire was designed with close ended questions and pre-piloted for
face validity by distributing it to 2 students of each study year. The comments and recommendations of
the students were considered in the final version of the questionnaire; however, their responses were not
included in the results. The study was carried out during April-June, 2019. The survey was distributed to
a total of 264 students at the end of their classes and 2 researchers explained the purpose of the study and
upon completion of filling the questionnaire collected the surveys. The average time to complete the survey
was 20 minutes. The students were informed that their voluntarily participation and filling the questionnaire
will be considered a form of an informed consent. The questionnaire was divided into four sections, the first
include questions with regard to demographic characteristics of the participants namely gender, ethnicity,
year of study and parents’ profession.
In the second section, the questions covered aspects on the attitude of the students towards antibiotics including; “Do you finish the course of antibiotic?”, “Do you stop the antibiotic once you feel better?”, “ Do you think that if taken too often, antibiotics are less likely to work in the future?”, “Do you store your antibiotic as mentioned in label?”, “Do you have leftover antibiotics at home?”, “Do you use leftover antibiotics without medical consultation?”, “Do you keep expired antibiotics ?”, “Do you usually check the expiry date of the antibiotic before taking it?”, “Do you read/follow the leaflet before start using antibiotic?” and “Do you use antibiotics prescribed for a member of your family?”. In addition, questions and statements were added such as “I usually know how antibiotics should be taken, even if I was given information about their use” and “Do you have a home pharmacy” and “Where it is placed”. The third section’s questions/statements were to evaluate the level of knowledge of students of the various aspects of antibiotics and bacterial resistance and included; “Do you know what is meant by antibiotic resistance?”, “Do you think misuse of antibiotics can lead to development of resistance?”, “What is your source of information on antibiotics and resistance?”, “Do you think antibiotics are effective against bacteria ?”, “Do you think antibiotics are effective against viruses?”, “The physician provides enough information on antibiotic use”, “The pharmacist provides enough information on antibiotic use”, “Do you think antibiotic resistance is a global problem?”, “Do you think poor drug quality leads to resistance?”, “Do you think under treatment with antibiotics leads to resistance?”, “Do you think over treatment with antibiotics leads to resistance?”, “How do you dispose of leftover and expired medications?”, “Do you think the consumption of products of animals treated with antibiotics can be a source of resistance?”, Do you think animal husbandry (antibiotic usage in animals) is a source of antibiotic resistance?, “I trust information I get from the physician” and “I trust the information I get from the pharmacist”. The fourth section explored the practice of using antibiotics among students “Have you used antibiotics in the past 12 months?”,” Do you finish the course of antibiotic?”, “Do you take antibiotics to prevent any disease (prophylactically)?”, “Do you save the remaining, leftover antibiotic for the next time when you get sick?”, “Do you regularly check on expiry date of in-home stored medicine?”, “Reason(s) for taken antibiotic”, “Do you take antibiotics for cold or sore throat?”, “Do you believe common colds are cured more quickly with antibiotics?”, “Do you take antibiotics for fever?”, “For how long do you usually take your antibiotic course?”, “Do you keep leftover (used) antibiotic (syrups, tablets, capsules, ear/eye drops ,ear/eye ointments )” and “Leftovers antibiotics should be returned back to the pharmacy”.
Data analysis was encoded on excel sheet and descriptive statistics were calculated by using SPSS (version
20). The data were summarized as frequencies and percentages. Comparison of responses of the three groups
of students and significant association between demographic characteristics of the participants and their
responses was determined at a level of significance set at p-value < 0.05.
Ethical Approval was obtained from the Ethical Committee of the University of Sharjah prior to conductance
of the study. The purpose of the study and confidentiality of the information were clarified to participants
and a written informed consent was obtained from each respondent before collection of data.
Results
The questionnaire was distributed to 264 students and a total of 241 completely filled in surveys were received
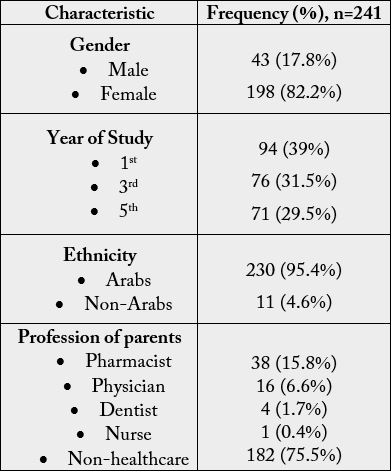
back producing a response rate of 91.3%. Table 1 shows that the majority (198, 82.2%) of respondents were
females, Arabs (230, 95.4%) and with parents of non-health care profession (182, 75.5%). Parents of the rest
of the participants were of health care professions.
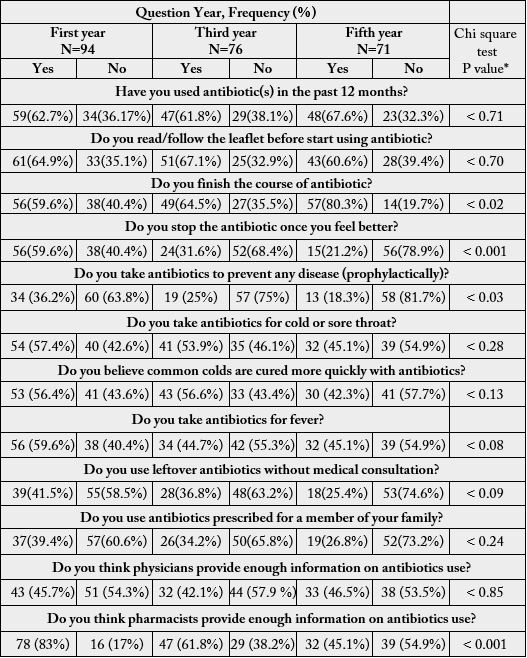
About two thirds (60-67%) of all students had used antibiotics in the last 12 months and they read the
instruction leaflet before using antibiotics (Table 2). Also shown in the same table that significantly (p <
0.02) more fifth (57, 80.3%) than first (56, 59.6%) and third (49, 64.5%) year students finish the course of
antibiotic, while more (p < 0.001) of both the advanced than the first year students do not stop the antibiotic
once they feel better and do not take antibiotics prophylactically to protect against diseases (p < 0.03).
*Significance P < 0.05
Students taking antibiotics for cold or sore throat comprised 54 (57.4%), 41 (53.9%) and 32 (45.1%) for first, third and fifth years respectively. Non-significantly (p< 0.08) more of first (56, 59.6%) than third or fifth year (40% and 45%) use antibiotics for fever, and about 25-40% of all students use leftover antibiotics without medical consultation and use antibiotics that are prescribed for other family members. Similar percentages (42-46%) of all students think that physicians provide more information on antibiotics while significantly (p < 0.001) more first (78, 83%) than third (47, 61.8%) or fifth (32, 45.1%) year students believe the pharmacist provides more information on antibiotics. Regarding the proper duration of use of antibiotics, the majority (69.7%) of female and only a few (7.4%) of male respondents selected 1-7 days, while 8.7% and 11.6% of male and female students selected a period of 1-14 days. A period of 21 days and more was selected by a negligible % of either group.
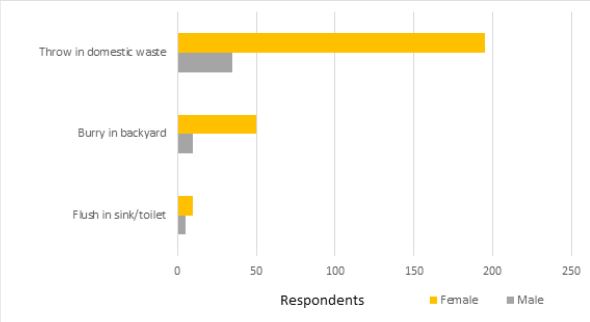
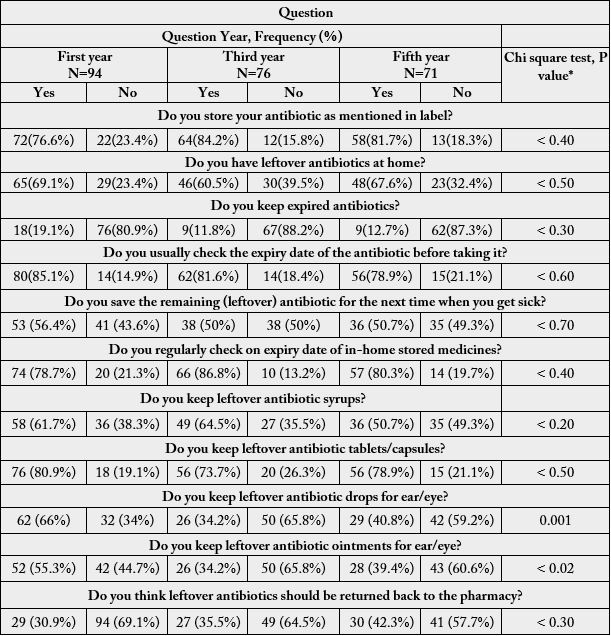
However, only small percentage (12-19%) of each group keeps expired antibiotics at home, while 79-85% of each group usually checks on the expiry date of kept antibiotics. About 50% of each group of students admitted storing leftover antibiotics for future use. Students who keep leftover antibiotics syrups and tablets/ capsules comprise 50-65% and 74-81% respectively. Significantly (p < 0.001 and p< 0.02) more first than third or fifth year students keep leftover ear/eye drops and ointments respectively and only 31-42% of each group think that leftover antibiotics should be returned to the pharmacy. Responses of male and female students to the question on their safe methods of disposal of expired antibiotics are shown in Fig. 1, while results of questions in-home storage of antibiotics are shown in Table 3.
*Significance P < 0.05
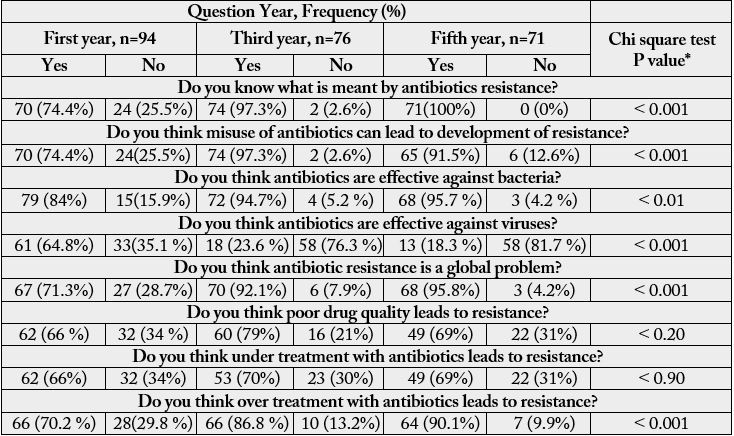
Responses of students to questions evaluating their knowledge are shown in Table 4. Significantly (p<
0.001) more third (74, 97.3) and fifth (71, 100%) than first (70, 74.4%) year students knew what is meant
by bacterial resistance and that misuse of antibiotics can lead to development of resistance. Again more
third and fifth than first year students knew that antibiotics are effective against bacteria (p< 0.01) but not
viruses (0.001). Those who believed that antibiotics are effective against viruses were about two thirds of first
(61, 64.8%) year students as compared to only 18 (23.6%) and 13 (18.3%) of third and fifth year students
respectively (p < 0/.001).
*Significance P < 0.05
With the exception of gender, no significant association was observed between other demographics and
students’ responses to various questions. Results of the influence of gender on some aspects of knowledge
of students on antibiotics are shown in Table 5. More male than female students know what is meant
by bacterial resistance (p< 0.05), know that antibiotics are effective against bacteria (p <0.02), do not use
antibiotics prophylactically (p< 0.05) and have a home pharmacy to store medications (p<0.01).

*Significance P < 0.05
Discussions
This study surveyed pharmacy students at the university of Sharjah-UAE to assess their knowledge, attitude
and use of antibiotics. The latter is progressively increasing in the country [12]. Among other factors that
enhance the emergence of resistant bacterial strains are under- and over- treatment with and the irrational
use of antibiotics in humans and animals [13]. The problem has recently been an alarming global concern. The
high prevalence of self-medication with antibiotics in UAE significantly contributes to bacterial resistance
[5]. The issue is aggravated by lack of knowledge and misconceptions on antibiotics. Most (82.2%) of the
participants were females. This reflects the common trend in colleges of health sciences in the UAE. About
two thirds of each group used antibiotics in the last 12 months. Knowledge of fifth year students although
better than that of third or first year, but in general seems poor when considering responses of the entire
groups of students that considered antibiotics to be effective in common cold, sore throat and fever which
are mostly due to viral infection. Such misconceptions are illustrated in 40-60% of the three study groups.
This result is in accordance with the observations in Malaysian and Chinese adults [14,15] but higher than
those for Saudi patients [16]. Results of the present study also indicated that significantly more fifth than
first or third year students finish their course of antibiotics and do not stop it once they feel better. Our
results also indicated that almost all third and fifth year know what is meant by bacterial resistance, are aware
that misuse of the drugs lead to bacterial resistance, that antibiotics are effective against bacteria but not
viruses and the problem of resistance is a global one as compared to first year students. However, only about
two thirds of each group were aware that poor drug quality and under treatment with antibiotics can lead to
resistance, while significantly more fifth and third year students than first year believed that over treatment
can also lead to resistance. Such behavior of advanced year students may be expected as at the level of their
study they gain reasonable level of knowledge through their pharmacology and microbiology courses. Only
small percentage of each group keep expired antibiotics at home. Such practice should not be encouraged as
the intentional or non-intentional use of expired medicines may lead to resistance as well as worsening of
the condition for which they are used. This is may be even worsened by the fact that 50% and more of each
group keep various formulations of leftover antibiotics for future use including syrups, ear/eye ointment and
drops which should be disposed of once the course of treatment is finished.
It has indeed been shown that sore throat; tonsillitis and similar conditions were frequently the causes of self-medicating with left over antibiotics [17-19]. It is worth noting that studies in medical students with low rates of antibiotic use, demonstrated that their consumption was irresponsible reflecting that their knowledge was not in harmony of their behavior [20]. When asked about duration of antibiotic use, more females than males selected 1-7 days, while almost similar but small numbers of both groups selected 1-14 days and very few males selected 1-21 days. Moreover, high percentages, about two thirds, of the three groups do not favor returning leftover antibiotics to pharmacy and more of both males and females throw expired antibiotics in domestic waste. In addition, studying the influence of gender on some aspects of knowledge of antibiotics, resistance and availability of home pharmacy indicated a significant association between gender and these aspects. Significantly more female than male students know the meaning of bacterial resistance, know that antibiotics are effective against bacteria, believe that under treatment with antibiotics can lead to bacterial resistance and have home pharmacy. On the other hand more male than female students know the meaning of bacterial resistance and use antibiotics prophylactically,
Results of the present study indicate that although students of advanced (third and fifth) years of study may have more knowledge of aspects of antibiotic use and bacterial resistance, there are gaps in such a knowledge and serious misconceptions when it comes to storage of left over and expired antibiotics and their use without medical consultation.
Conclusion and Recommendations
Since all health authorities are aware of the seriousness of the global problem of the irrational use of
antibiotics and the emergence of bacterial resistance, it is rather imperative to suggest that intensive focus
should be directed on educational courses and programs directed to university students. Focus on students
of health sciences colleges including medical, dental, pharmacy, nursing and other health related specialties
would certainly equip them with more knowledge and skills to educate the public as future health care
provider. Also continuing education programs stressing on responsible use of antibiotics should target all
health care professionals.
Limitations
The present study focused on pharmacy students of only one university in UAE, therefore the results cannot
be generalized.
Bibliography

Hi!
We're here to answer your questions!
Send us a message via Whatsapp, and we'll reply the moment we're available!