Biography
Interests
Christine Carroll1* & Jeff Guthrie, A.2
1Emergency Medicine Physician, Bayne Jones Army Community Hospital, Fort Polk, Louisiana
2Chief of Department of Radiology, Bayne Jones Army Community Hospital, Fort Polk, Louisiana
*Correspondence to: Dr. Christine Carroll, Emergency Medicine Physician, Bayne Jones Army Community Hospital, Fort Polk, Louisiana.
Copyright © 2021 Dr. Christine Carroll, et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
In cases of chronic abdominal pain in geriatric population a high index of suspicion needs to be maintained to gather data that would determine the emergency physician arrive to a diagnosis for appropriate patient management and referrals to the appropriate services. We present the case of an elderly patient who arrived at our Emergency Department after multiple visits for chronic abdominal pain and weight loss. She had an extensive prior workup that excluded malignancy and other overt etiologies yet she remained undiagnosed. Previous imaging did note severe atherosclerotic vascular disease, including severe narrowing of the celiac, superior mesenteric and inferior mesenteric arteries. Combing this information with a detailed history yielded the diagnosis of chronic mesenteric ischemia. This case should alert physicians that listening closely to the patient and combining that information with all available testing data may lead them to the correct diagnosis in complicated cases. This is especially important in situations when patients have prior negative workups with no findings but report continued worsening of their condition.
Introduction
Chronic mesenteric ischemia (CMI) also known as intestinal angina is an uncommon condition that if
diagnosed with delay can evolve to intestinal infarction [1-5]. It represents approximately 1-2% of all the
abdominal diseases with an annual incidence of about 1/100,000 in the older population with women
affected more than men [1,2,4].
Constant or intermittent intestinal hypoperfusion secondary to atherosclerosis causing stenosis or occlusion of at least two visceral arteries may be the cause in 90% of the cases [1,2,4,5]. Almost 18% of people over 65 may have significant stenosis of the superior mesenteric artery (SMA) or celiac trunk and they may have no symptoms thus making diagnosis difficult [1,5]. However, because of extensive collateral circulation patients may not develop symptoms until late in the disease process [3,5]. At that point in time, if the intestinal blood flow is unable to meet the metabolic demands of the gut, ischemia may develop because the oxygen and nutrient delivery is not sufficient to meet the demands of cellular metabolism [1,3].
The most common symptoms are unexplained chronic abdominal pain, weight loss and fear of eating [1,2,4,5]. 87% of patients usually complain of dull, crampy, postprandial epigastric pain with radiation to the back within one hour after eating that subsides within two to six hours [1,2].
Case Report
An 85 year old female with history of hypertension (HTN) presented to the Emergency Department (ED)
with a 30lbs weight loss and persistent mid-epigastric pain for a fourth visit over the span of six months. The
epigastric pain was postprandial and intermittently radiated to the back. The post prandial pain was initially
present just with solids, then it also occurred with liquids. It worsened to a point that patient developed
fear of eating in anticipation of intense pain. On presentation patient was cachectic looking with normal
vitals. Abdomen was soft, scaphoid with mild tenderness to midepigastric area, normal bowel sounds and
no pulsatile masses. Labs were unremarkable other than mildly elevated lipase 100U/L (normal 8-78 U/L).
Thyroid function, complete blood count, complete metabolic panel, troponin, lactate and urinalysis were all
unremarkable. EKG had no abnormal T waves, no ST segment elevations or depressions. She underwent
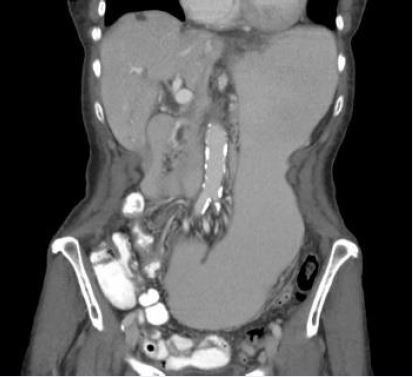
a CT abdomen and pelvis with IV and oral contrast which revealed severe diffuse atherosclerotic vascular
disease at the origin of the celiac trunk and SMA as well as profound gastric dilatation which was not
present on another CT only 4 days prior. The radiologist recommended an upper GI fluoroscopic exam
based on the found gastric dilatation (fig. 1). The exam was performed the next day and remarkable only for
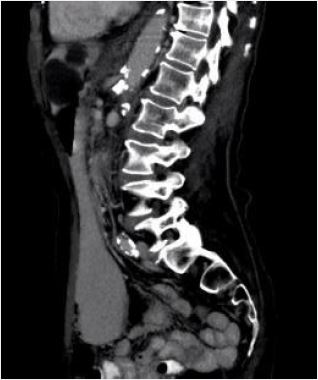
resolution of the gastric dilatation. An abdominal CT was performed and confirmed severe arterial disease
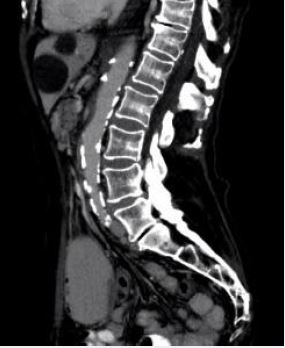
with severely narrowed celiac trunk (fig. 2) and complete occlusion of the SMA (fig. 3), findings that were
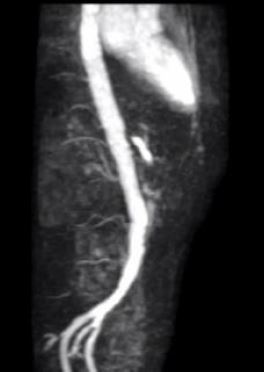
later confirmed by the magnetic resonance angiography (MRA). She had extensive collateral circulation
coming from the iliac arteries, left hepatic artery and left lumbar artery (fig. 4). She was transferred to a
tertiary care center for vascular and general surgery evaluation for endovascular treatment and jejunostomy
respectively. Patient had one more visit to our ED for epigastric pain before being evaluated at the tertiary
care center. She was then lost to follow up.
Discussion
Because of the unspecific symptoms of CMI, some patients suffer of chronic abdominal pain with severe
malnutrition and bowel necrosis before the correct diagnosis is made [5,6]. Timely diagnosis is often delayed
by 10.7 to 15 months because patients may be initially evaluated for other causes of weight loss [1,6].
Therefore a high clinical suspicion needs adopted in caring for patients with atherosclerosis, HTN, cardiac
disease or peripheral arterial disease [6].
The diagnostic process often requires multiple radiologic procedures and involvement of several surgical and medical disciplines [2,4]. Imaging may involve an initial duplex ultrasonography, and, if inconclusive, CT angiography (CTA) or MRA [1,4,5]. However, CTA may be the best initial imaging modality since it not only defines presence of atherosclerotic plaque, but it can also help rule out other intra-abdominal pathology [1]. Once CMI is diagnosed, patients must undergo mesenteric angioplasty and stenting using either open or endovascular techniques since conservative treatments such as bowel resting, smoking cessation and vasodilator drugs do not stop disease progression or ameliorate symptoms [1,2,4].
Routine follow up is recommended for open or endovascular treatment for CMI in order to identify recurrent symptoms and restenosis [1]. End point of treatment is remission of symptoms defined as complete cessation of postprandial pain and weight gain >5kg [3].
In this case of CMI, the emergency team made efforts to proceed with additional studies while the patient was in the ED. In addition, the team consulted general surgery early in the process which also expedited the diagnosis. This report serves as a reminder of many basic tenets of medicine including the importance of thorough history taking, the utility of a multidisciplinary team in complicated cases and the need to broaden the differential diagnosis for patients with continued presentations for common symptoms but no readily identifiable etiology.
Conclusion
Routine follow up is recommended for open or endovascular treatment for CMI in order to identify recurrent
symptoms and restenosis [1]. End point of treatment is remission of symptoms defined as complete cessation
of postprandial pain and weight gain >5kg [3].
In this case of CMI, the emergency team made efforts to proceed with additional studies while the patient was still in the ED. In addition, the team got general surgery involved in the case early in the process. Because of the severely narrowed celiac trunk and complete occlusion of both SMA and IMA, the patient was referred to general surgery and vascular surgery for endovascular treatment and jejunostomy for nutritional needs to rehabilitation. At the first surgery visit the team decided she had a jejunostomy first because of her profound weight loss and concerns she may have surgical complications secondary to that. After that visit patient follow up was lost since she did not have any more visits in our system.
Through this report a suggestion is made for attempting to obtain a thorough exam and additional imaging along with appropriate follow up for a definitive diagnosis that would ultimately improve the patient’s outcome.
Bibliography

Hi!
We're here to answer your questions!
Send us a message via Whatsapp, and we'll reply the moment we're available!